Key Takeaways
- Waking up at night is normal, but struggling to fall back asleep (maintenance insomnia) can disrupt your sleep cycle and overall health
- Your racing mind is the primary culprit – anxiety about not sleeping creates a frustrating cycle that keeps you awake longer
- The 4-7-8 breathing technique and the counterintuitive “get out of bed” strategy are proven methods to help you fall back asleep faster
- Creating an optimal sleep environment with proper temperature (60-67°F), minimal light, and comfortable bedding significantly impacts your ability to stay asleep
You jolt awake at 2 AM, eyes wide open, mind suddenly racing. What now?

That frustrating middle-of-the-night awakening isn’t just annoying—it’s a common form of insomnia that affects nearly 20% of people with sleep troubles. The technical term is “sleep maintenance insomnia,” and it describes the inability to stay asleep throughout the night. While occasional wake-ups are completely normal, the real problem begins when you can’t drift back to dreamland.
SleepReset, understands the frustration of staring at the ceiling while minutes turn to hours. Their sleep coaches work with clients every day who struggle with this exact issue. The good news? With the right approach, you can break this cycle and return to restful, uninterrupted sleep.
Why You’re Stuck Awake at 2 AM: Understanding Nighttime Awakenings
Before searching for solutions, it helps to understand why your sleep keeps breaking. Contrary to popular belief, humans aren’t naturally programmed to sleep in one continuous block. Historically, our ancestors likely slept in segments, with periods of wakefulness in between. However, in our modern world, these wake periods have become problematic when they stretch from minutes into hours.
Several factors contribute to these extended awakenings. Your body’s natural sleep cycles move through different stages approximately every 90 minutes. During lighter sleep phases, you’re more susceptible to awakening from environmental triggers, physical discomfort, or mental activity. What determines whether you fall right back asleep or lie awake for hours often comes down to what happens in those first few minutes after opening your eyes.
- Environmental disruptions (noise, light, temperature changes)
- Physical discomfort (pain, fullness, need to use the bathroom)
- Stress and anxiety (work concerns, relationship issues)
- Hormonal fluctuations (especially in women)
- Sleep disorders (sleep apnea, restless leg syndrome)
- Certain medications or substances (alcohol, caffeine)
Understanding your specific triggers is the first step toward addressing the problem. Many people find that keeping a sleep journal helps identify patterns and potential causes of their nighttime awakenings. For more insights on how to go back to sleep after waking up, you can explore various strategies and tips.
The Sleep Cycle Disruption
Your sleep isn’t just one long state of unconsciousness—it’s a complex rhythm of different stages.
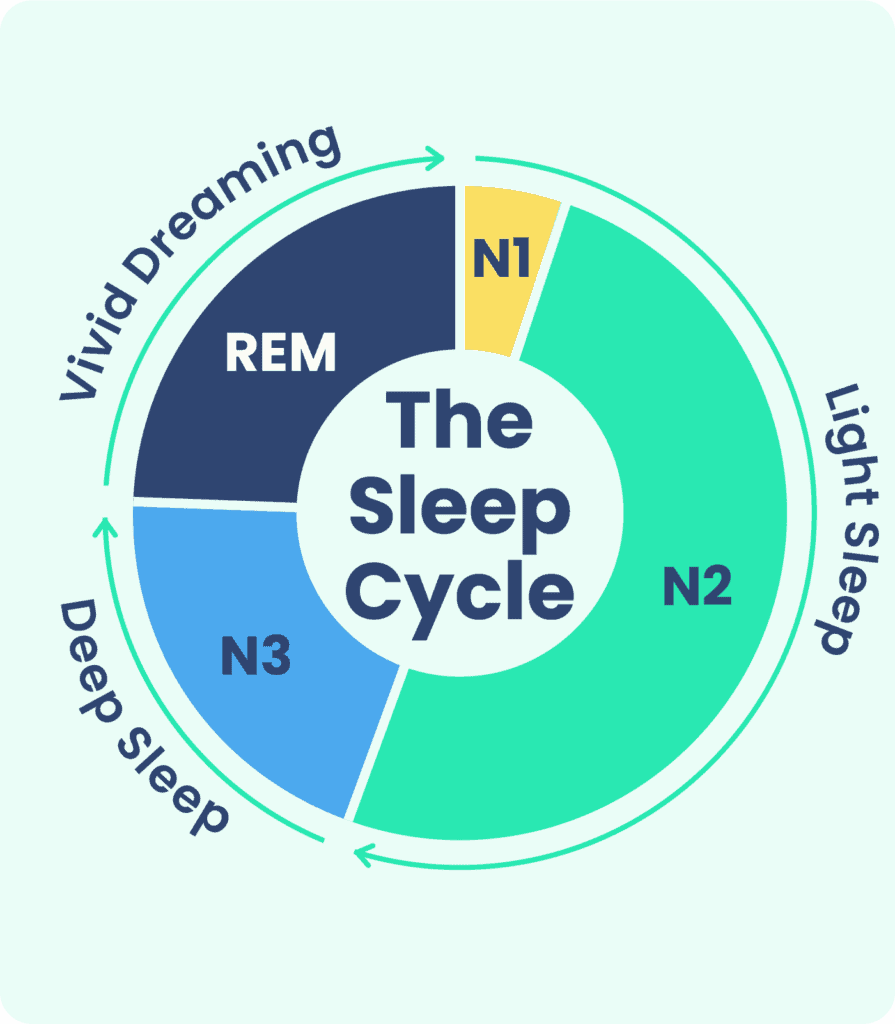
“What Happens in a Normal Sleep Cycle …” from www.sleepfoundation.org
Throughout the night, you cycle through light sleep, deep sleep, and REM (rapid eye movement) sleep. Each cycle typically lasts about 90 minutes, meaning you’ll complete 4-6 cycles during an average night’s sleep.
When you wake up during one of these cycles, particularly during lighter stages of sleep, your brain can easily shift into alert mode. Once fully awake, many people make the situation worse by checking the time, which can trigger anxiety about how much sleep they’re losing. This anxiety activates your sympathetic nervous system—the “fight or flight” response—making it physiologically more difficult to fall back asleep. To understand more about the causes of insomnia, it’s important to consider how these physiological responses affect sleep.
Common Triggers That Keep You Awake
Most middle-of-night awakenings start innocently enough. Perhaps you heard a noise, needed to use the bathroom, or simply shifted between sleep cycles. What transforms these normal wake-ups into prolonged periods of insomnia often comes down to what happens next. For some, issues like nighttime GERD (indigestion) can further complicate getting back to sleep.
The most common culprit is cognitive arousal—when your mind begins processing thoughts, worries, or even just awareness of being awake. This mental activity can quickly escalate, especially if you start worrying about not getting enough sleep. Physical discomfort from pain, temperature issues, or hunger can also keep you awake. Environmental factors like light leaking through your blinds, your partner’s snoring, or ambient noise can make it difficult to drift off again.
Additionally, what you did before bed matters significantly. Consuming alcohol might help you fall asleep initially, but it disrupts your sleep architecture and often leads to middle-of-night awakenings as your body metabolizes the alcohol. Similarly, late caffeine consumption, heavy meals, or intense exercise close to bedtime can all contribute to sleep maintenance problems.
The Negative Thought Spiral
“I can’t fall back asleep” → “I’ll be exhausted tomorrow” → “I won’t perform well at work” → “My job could be at risk” → “I need to sleep NOW” → Increased anxiety → Even more difficulty sleeping
Why Your Brain Won’t Shut Off
The most frustrating aspect of nighttime awakenings is often the racing mind that accompanies them. One moment you’re peacefully asleep, and the next your brain is running through tomorrow’s meeting agenda, replaying an awkward conversation from five years ago, or spiraling through worst-case scenarios about your health, relationships, or finances.
This mental hyperactivity stems from several factors. First, your prefrontal cortex—responsible for logical thinking and decision-making—becomes more active during these awakenings. Without the distractions of daytime life, these thoughts can seem louder and more persistent. Second, anxiety about being awake creates a self-perpetuating cycle: you worry about not sleeping, which produces stress hormones like cortisol, which further prevents sleep. Learn more about what happens in your brain to cause insomnia.
Understanding that this is a normal physiological response, not a personal failing, is the first step toward breaking the cycle. Your brain isn’t broken—it’s just doing what brains sometimes do in the quiet darkness of night.
5 Immediate Actions to Fall Back Asleep Fast
When you find yourself wide awake in the middle of the night, your initial response matters tremendously. The right approach can ease you back to sleep within minutes, while the wrong one might keep you up for hours. Here are five research-backed techniques you can implement immediately the next time sleep eludes you.
1. The 4-7-8 Breathing Technique
This powerful breathing method acts as a natural tranquilizer for your nervous system. Developed by Dr. Andrew Weil, it’s based on ancient yogic practices that help calm the mind and relax the body. The technique is simple: inhale quietly through your nose for 4 seconds, hold your breath for 7 seconds, then exhale completely through your mouth for 8 seconds, making a whooshing sound. Repeat this cycle 3-4 times.
The 4-7-8 technique works by increasing oxygen in your bloodstream, slowing your heart rate, and releasing carbon dioxide from your lungs. This physiological shift helps counteract the stress response that often keeps you alert during nighttime awakenings. Many SleepReset clients report that this technique helps them fall back asleep within minutes, even after previously struggling with hour-long wake periods. For additional insights on what happens in your brain during these wakeful periods, check out what happens in your brain to cause insomnia.
2. Get Out of Bed (Counterintuitive But Effective)
This strategy seems counterproductive but is supported by substantial research. If you’ve been awake for more than 20 minutes, sleep experts recommend getting out of bed entirely. Move to another room, keep lights dim, and engage in a quiet, non-stimulating activity like reading a physical book (not an e-reader) or listening to calming music. Only return to bed when you feel genuinely sleepy again.
This approach works by preventing your brain from creating an association between your bed and wakefulness. The longer you lie in bed frustrated and awake, the stronger this negative association becomes. By removing yourself until sleepiness returns, you maintain your bed as a place exclusively for sleep, strengthening the bed-sleep connection in your brain.
3. Body Scan Relaxation
The body scan technique helps quiet your mind by redirecting attention to physical sensations rather than racing thoughts. Starting at your toes, systematically focus your attention on each part of your body, moving upward. As you concentrate on each area, consciously release any tension you notice. This mindfulness practice not only relaxes your muscles but also interrupts ruminating thought patterns that keep you alert.
Many people find it helpful to pair this technique with slow, deep breathing. The combination creates a powerful relaxation response that can significantly increase your chances of drifting back to sleep. This method is particularly effective for those whose nighttime awakenings are characterized by physical tension or anxiety-related bodily sensations.
4. Adjust Your Sleep Environment
Sometimes, environmental factors are keeping you awake without you realizing it. If you wake up and can’t fall back asleep, take a moment to assess your surroundings. Is your room too hot or cold? Is light seeping in from somewhere? Can you hear disruptive noises? Making quick adjustments to temperature, light, or sound can sometimes solve the problem immediately.
Keep a sleep mask, earplugs, or a white noise machine within easy reach to address these issues without fully disrupting your sleep state. Even small environmental tweaks can signal to your body that conditions are right for continued sleep. Remember that your sleep environment should remain consistently conducive to sleep throughout the entire night, not just when you initially go to bed.
5. Try the Military Method
Developed to help soldiers fall asleep in challenging conditions, this technique can work wonders for middle-of-night awakenings. Start by relaxing your entire face, including the muscles inside your mouth. Drop your shoulders to release tension and let your hands fall naturally to the sides of your body. Exhale slowly, relaxing your chest, then relax your legs, starting from the thighs and working down.
After physically relaxing, spend 10 seconds trying to clear your mind by imagining a relaxing scene. If that doesn’t work, try repeating the phrase “don’t think” over and over for 10 seconds. This method typically works by mentally and physically relaxing you, often leading to sleep within 10-120 seconds. With practice, many people find it becomes increasingly effective over time.
Break the Cycle: Preventing Middle-of-Night Insomnia
Evening Routine Adjustments
What you do in the hours before bedtime significantly impacts your ability to maintain continuous sleep throughout the night. Creating a consistent wind-down routine signals to your brain that it’s time to prepare for rest. Ideally, this routine should begin 30-60 minutes before your intended sleep time and include calming activities that help transition from daytime alertness to nighttime restfulness.
The key is consistency—performing the same relaxing activities in the same order each night creates powerful mental associations. Your brain begins to recognize these cues and initiates sleep-promoting processes in response. This predictability helps stabilize your circadian rhythm, which in turn reduces the likelihood and duration of nighttime awakenings.
- Take a warm bath or shower (the subsequent cooling effect promotes sleepiness)
- Practice gentle stretching or yoga poses designed for relaxation
- Write in a journal to transfer worries from your mind to paper
- Read something calming and non-stimulating (avoid thrillers or work material)
- Listen to sleep-inducing music or nature sounds
Remember that your evening routine doesn’t need to be elaborate—even simple consistent habits can make a profound difference. At SleepReset, our coaches work with clients to develop personalized evening routines that fit their lifestyle while maximizing sleep-promoting benefits. We’ve found that even small adjustments often yield significant improvements in sleep maintenance.
Digital Device Boundaries
The blue light emitted by phones, tablets, computers, and TVs interferes with your production of melatonin, the hormone that regulates your sleep-wake cycle. This disruption makes it harder both to fall asleep initially and to maintain sleep throughout the night. Establish a technology curfew at least 60 minutes before bedtime, and keep devices out of the bedroom entirely if possible. If you use your phone as an alarm, consider purchasing a dedicated alarm clock instead, allowing you to charge your phone in another room overnight.
Food and Drink Timing
What and when you consume food and beverages can significantly impact your sleep quality. Aim to finish eating at least 2-3 hours before bedtime to allow for proper digestion. Heavy meals, spicy foods, and high-fat items require more time to digest and can cause discomfort that interrupts sleep. Similarly, limit liquids in the hours before bed to reduce the likelihood of bathroom trips interrupting your night. Most importantly, monitor your caffeine and alcohol consumption—caffeine has a half-life of 5-6 hours and can disrupt sleep even when consumed early in the afternoon, while alcohol might help you fall asleep initially but often leads to fragmented, poor-quality sleep as your body metabolizes it throughout the night.
finish eating at least 2-3 hours before bedtime to allow for proper digestion. Heavy meals, spicy foods, and high-fat items require more time to digest and can cause discomfort that interrupts sleep.

The Hidden Health Factors Keeping You Awake
Sometimes persistent middle-of-night awakenings stem from underlying health conditions that might not be immediately obvious. Addressing these root causes often resolves sleep maintenance issues more effectively than treating the insomnia directly. Your body might be trying to tell you something important through these disrupted sleep patterns, such as nighttime GERD.
Chronic pain conditions frequently manifest as sleep disturbances, with pain signals intensifying during the relative quiet of nighttime. Gastrointestinal issues like acid reflux can worsen when lying down, triggering awakenings. Even mild respiratory problems such as allergies or slight airway restrictions can disrupt your sleep cycle without fully waking you, leaving you with fragmented, non-restorative sleep.
- Untreated sleep apnea or upper airway resistance syndrome
- Hormonal imbalances (thyroid issues, menopause, low testosterone)
- Chronic pain conditions (arthritis, fibromyalgia, back pain)
- Medication side effects or interactions
- Gastrointestinal disorders like GERD or IBS
- Mental health conditions (depression, anxiety disorders, PTSD)
Tracking your symptoms alongside your sleep patterns can help identify correlations that might point to underlying health issues. Note any patterns in when awakenings occur, what symptoms accompany them, and any factors that seem to make them better or worse. This information becomes invaluable when consulting healthcare providers.
At SleepReset, we emphasize a holistic approach to sleep health that considers these underlying factors rather than just treating the surface-level symptoms of insomnia.
Stress and Anxiety Impacts
Psychological factors play a profound role in sleep maintenance problems. Your mind and body are intrinsically connected through complex neurological and hormonal pathways, with stress and anxiety being particularly disruptive to sleep architecture. When you experience chronic stress, your body produces elevated levels of cortisol, the primary stress hormone. This biochemical change directly interferes with your sleep-wake cycles and can lead to frequent nighttime awakenings. For more insight into how stress affects your sleep, explore what happens in your brain to cause insomnia.
Hormonal Influences
Hormonal fluctuations throughout life significantly impact sleep patterns, often in ways that aren’t immediately obvious. Women frequently report increased sleep disturbances during menstruation, pregnancy, and perimenopause due to changing levels of estrogen and progesterone. Similarly, men experiencing age-related testosterone decline often develop sleep maintenance problems. Thyroid imbalances—both hypothyroidism and hyperthyroidism—commonly manifest as sleep disturbances, including middle-of-night awakenings.
Sleep Disorders That Cause Fragmented Sleep
Sometimes what feels like simple insomnia might actually be a specific sleep disorder requiring targeted treatment. Sleep apnea, characterized by breathing interruptions during sleep, can cause multiple awakenings that you might not fully remember but that nonetheless fragment your sleep. Restless leg syndrome and periodic limb movement disorder create uncomfortable sensations or movements that disrupt sleep cycles. Circadian rhythm disorders can cause misalignment between your internal clock and environmental cues, leading to sleep maintenance difficulties.
Your Sleep Environment Matters More Than You Think
The conditions of your bedroom play a crucial role in maintaining continuous sleep throughout the night. Even small environmental disruptions can trigger awakenings or prevent you from easily falling back asleep. Creating an optimal sleep sanctuary involves attention to several key elements that signal to your brain and body that it’s time for rest.
Studies show that environmental factors account for approximately 40% of sleep quality variations between individuals with similar health profiles. Investing time and resources into optimizing your sleep environment often yields significant improvements in sleep maintenance with minimal effort. This approach represents one of the most accessible and effective interventions for reducing nighttime awakenings.
Temperature Control for Better Sleep
Your body temperature naturally drops as part of the sleep process, and environmental temperature plays a crucial role in facilitating this decline. Most sleep experts recommend keeping your bedroom between 60-67°F (15-19°C) for optimal sleep. Temperatures outside this range can trigger awakenings as your body struggles to maintain its ideal sleep temperature.
Light and Noise Management
Even minimal light exposure during sleep can suppress melatonin production and disrupt your circadian rhythm. Install blackout curtains, remove electronic devices with LED indicators, or use a comfortable sleep mask to create complete darkness. Similarly, intermittent noises—even those not loud enough to fully wake you—can cause sleep fragmentation and reduce sleep quality. Consider using a white noise machine or app to create consistent background sound that masks disruptive noises and signals to your brain that sleep conditions remain stable throughout the night.
Bedding and Mattress Considerations
Your sleeping surface directly impacts your comfort and ability to maintain sleep throughout the night. An old or unsuitable mattress can cause pressure points and discomfort that trigger awakenings. Similarly, bedding that causes overheating or doesn’t properly support your sleeping position can lead to disrupted sleep. Invest in a high-quality mattress appropriate for your sleep position and preferences, along with breathable, comfortable bedding that helps regulate temperature throughout the night.
When to Seek Professional Help
While occasional sleep disruptions are normal, persistent problems with maintaining sleep warrant professional attention. If you’ve consistently struggled with middle-of-night awakenings for more than three weeks despite implementing good sleep hygiene practices, it’s time to consult a healthcare provider. Sleep disturbances can be both a symptom and a cause of other health issues, creating a complex relationship that benefits from expert guidance. For example, what happens in your brain to cause insomnia can be an underlying factor that needs addressing.
Don’t dismiss chronic sleep maintenance issues as “just insomnia” or an inevitable part of aging. Quality sleep remains essential throughout life, and effective treatments exist for most sleep disorders. Many people suffer needlessly for years before seeking help that could dramatically improve both their sleep and overall quality of life.
- Sleep disruptions occurring 3+ nights weekly for more than three weeks
- Daytime symptoms including excessive sleepiness, irritability, or difficulty concentrating
- Sleep problems accompanied by other health symptoms like snoring, gasping, or physical discomfort
- Sleep issues causing significant distress or impairing daily functioning
- Increasing reliance on sleep aids or alcohol to maintain sleep
Start with your primary care physician, who can assess for underlying medical conditions and provide referrals to specialists if needed. Come prepared with a sleep diary documenting your patterns over at least two weeks, including bedtimes, wake times, nighttime awakenings, and any factors that seem to influence your sleep quality.
At SleepReset, we often work collaboratively with medical providers to address sleep maintenance insomnia from multiple angles, combining behavioral approaches with appropriate medical interventions when necessary.
Warning Signs of a Serious Sleep Problem
While difficulty maintaining sleep is frustrating on its own, certain symptoms warrant more urgent medical attention. Seek immediate help if you experience severe gasping or choking sensations that wake you, as these may indicate obstructive sleep apnea—a serious condition linked to cardiovascular problems when left untreated. Similarly, extreme daytime sleepiness that interferes with driving or other essential activities requires prompt evaluation, as does any sudden onset of severe insomnia, particularly when accompanied by other neurological symptoms.
Types of Sleep Specialists
Several types of healthcare providers specialize in sleep medicine, each offering different perspectives and treatment approaches. Sleep medicine physicians complete specialized training in sleep disorders and often oversee sleep labs where diagnostic testing occurs. These doctors may come from various backgrounds including pulmonology, neurology, psychiatry, or internal medicine, each bringing unique expertise to sleep problems.
Behavioral sleep medicine specialists—often psychologists or therapists with specialized training—focus on non-medication approaches like cognitive behavioral therapy for insomnia (CBT-I), which has shown remarkable effectiveness for sleep maintenance problems. Sleep coaches or educators provide support for implementing behavioral changes and sleep hygiene practices, often working alongside medical providers to reinforce treatment plans.
What to Expect at a Sleep Consultation
A comprehensive sleep evaluation typically begins with a detailed history of your sleep patterns, health conditions, medication use, and lifestyle factors. The provider will likely ask about your sleep environment, evening routines, and any symptoms you experience during both day and night. Depending on your specific symptoms, they may recommend a sleep study (polysomnography) either in a lab setting or at home using portable monitoring equipment.
Based on this evaluation, the specialist will develop a treatment plan tailored to your specific sleep issues. This might include behavioral interventions, environmental modifications, medication adjustments, or treatment for underlying conditions. Follow-up appointments allow for monitoring progress and refining the approach as needed. The most effective treatment often combines multiple strategies rather than relying on a single intervention.
Back to Restful Nights: Recovery Timeline
Recovering from chronic sleep maintenance insomnia doesn’t happen overnight, but improvement often begins sooner than you might expect. Many people notice initial changes within the first week of implementing comprehensive sleep strategies, particularly those addressing behavioral patterns and sleep environment. However, complete resolution of long-standing sleep maintenance problems typically takes 4-8 weeks as your body readjusts to healthier sleep patterns and your brain forms new associations with sleep.
Consistency is crucial during this recovery period. Maintaining regular sleep-wake times, even on weekends, helps stabilize your circadian rhythm and improve sleep maintenance. Expect some fluctuations in progress—occasional difficult nights are normal and don’t indicate failure of your overall approach. The general trajectory matters more than any individual night’s sleep quality. With persistence and the right combination of strategies, most people can significantly reduce or eliminate problematic middle-of-night awakenings and return to restorative, continuous sleep. For more insights, explore the causes of sleep deprivation at night and find effective solutions.
Frequently Asked Questions
The following questions address common concerns about nighttime awakenings and provide evidence-based answers to help you better understand and address sleep maintenance insomnia.
Is it normal to wake up every night at the same time?
Waking at the same time night after night often relates to your circadian rhythm and sleep cycles. Each sleep cycle lasts approximately 90 minutes, and you’re more likely to awaken during lighter stages that occur at predictable intervals. Additionally, your body’s internal clock influences hormonal fluctuations throughout the night. For example, cortisol levels naturally rise in the early morning hours, which can trigger awakening around 3-4 AM for many people.
Consistent same-time awakenings might also relate to environmental cues like a partner’s movements, regular neighborhood noises, or subtle light changes. While occasional awakenings are normal, consistently waking and struggling to return to sleep warrants attention to both the timing and potential triggers.
How long should it take to fall back asleep after waking up?
For most people with healthy sleep patterns, returning to sleep after a brief nighttime awakening should take less than 20 minutes. This timeframe represents a general guideline rather than a strict rule, as individual variations exist.
Expected Return-to-Sleep Timeframes
Under 20 minutes: Normal range for most healthy sleepers
20-60 minutes: Occasional instances are normal, but regular occurrences suggest mild sleep maintenance issues
Over 60 minutes: Indicates significant sleep maintenance insomnia requiring intervention
Multiple hours or inability to return to sleep: Severe insomnia that warrants professional consultation
If you consistently require more than 20-30 minutes to fall back asleep after waking, implementing the techniques described earlier in this article can help reduce this return-to-sleep latency. The 20-minute threshold also serves as a useful decision point for whether to stay in bed (if feeling drowsy and relaxed) or temporarily get up (if feeling alert or anxious).
Remember that your perception of time often becomes distorted during nighttime awakenings—what feels like hours might actually be much shorter. Avoid checking the clock, as time-monitoring tends to increase sleep-related anxiety and extend wakefulness.
Can melatonin supplements help with middle-of-night awakenings?
Melatonin supplements can be helpful for sleep onset insomnia (difficulty falling asleep initially) but show mixed results for sleep maintenance problems. Standard melatonin supplements typically have a short half-life of 2-3 hours, meaning their effects may wear off during the night. For middle-of-night awakenings, extended-release formulations that provide a slower, more consistent release of melatonin throughout the night may prove more beneficial.
When considering melatonin, timing matters significantly. For sleep maintenance issues, taking it 1-2 hours before bedtime works best, allowing levels to peak as you fall asleep and maintain presence throughout the night. Start with a low dose (0.5-1mg) and increase gradually if needed, as higher doses don’t necessarily improve effectiveness and may cause side effects like morning grogginess or headaches. Always consult with a healthcare provider before starting any supplement regimen, especially if you take other medications or have underlying health conditions.
Will sleeping pills help me stay asleep through the night?
Prescription sleep medications can effectively reduce nighttime awakenings in the short term, but they come with significant limitations and concerns. Most sleep medications alter your natural sleep architecture, potentially reducing time spent in deeper, more restorative sleep stages while increasing lighter sleep. This trade-off means you might sleep continuously but wake feeling less refreshed. Additionally, many sleep medications carry risks of dependency, tolerance (requiring increasing doses for the same effect), and rebound insomnia when discontinued. For these reasons, most sleep specialists recommend prescription sleep aids only for short-term use while developing more sustainable behavioral approaches to address the underlying causes of sleep maintenance insomnia.
Does the “sleep when you’re tired” approach work for fixing sleep maintenance insomnia?
The “sleep when you’re tired” approach, while intuitive, generally proves counterproductive for resolving sleep maintenance insomnia. This method, which involves going to bed only when feeling sleepy and waking naturally without an alarm, can work well for people with minimal sleep issues. However, for those with established sleep maintenance problems, this inconsistent scheduling can further disrupt your circadian rhythm and exacerbate sleep difficulties.
Research consistently shows that maintaining regular sleep-wake times—even on weekends—helps stabilize your body’s internal clock and improve sleep continuity. This regularity strengthens the circadian signals that promote consolidated sleep throughout the night. While it’s important to align your bedtime with your natural tendencies (whether you’re naturally an early bird or night owl), consistency within that pattern matters most for overcoming sleep maintenance issues.
The most effective approach combines consistency with proper sleep timing. Go to bed when you’re likely to fall asleep within 20-30 minutes, wake at the same time daily, and maintain this schedule regardless of sleep quality on any particular night. This consistency reinforces your body’s natural sleep-wake rhythm and gradually improves your ability to maintain continuous sleep.
If you’re struggling with persistent sleep maintenance insomnia, don’t face it alone. SleepReset offers personalized coaching and evidence-based approaches to help you reclaim your nights and wake up feeling truly rested.
Many people struggle with sleep deprivation at night, finding it difficult to fall back asleep after waking up. This can be due to various reasons such as stress, anxiety, or even physical discomfort. Understanding the causes of sleep deprivation can help in finding effective solutions to improve sleep quality and ensure a restful night.
